America’s health care system provides some of the finest doctors and more access to vital medications than any country in the world. And yet, our system has been faltering for many years with the increased cost of health care.
Almost every economist agrees that the American health care system is unsustainable. Medical care is so expensive that it is busting all of our budgets – government, business, and personal. Eventually, the medical price bubble will pop. What, then, are the alternatives?
VITAL, BUT OUT OF CONTROL
Universal access to decent medical care has long been recognized as a worthy goal for any decent society to pursue. This functions as an important form of insurance for average people, who often lack the financial reserves needed to weather an unpredictable medical crisis. Given the nature of infectious disease, it is also a matter of public safety.
Yet rising medical costs remain an issue across the Western world. Medical debt is the second most significant form of debt in the U.S. One in five Americans are burdened with it. Indeed, in a 2017 Gallup survey, over 50% of Americans revealed being worried about health care costs Gallup. Similarly, in the EU, 22% of those surveyed found it difficult to cover expenses for specific health care services and felt strong insecurity about the near future Eurofound.
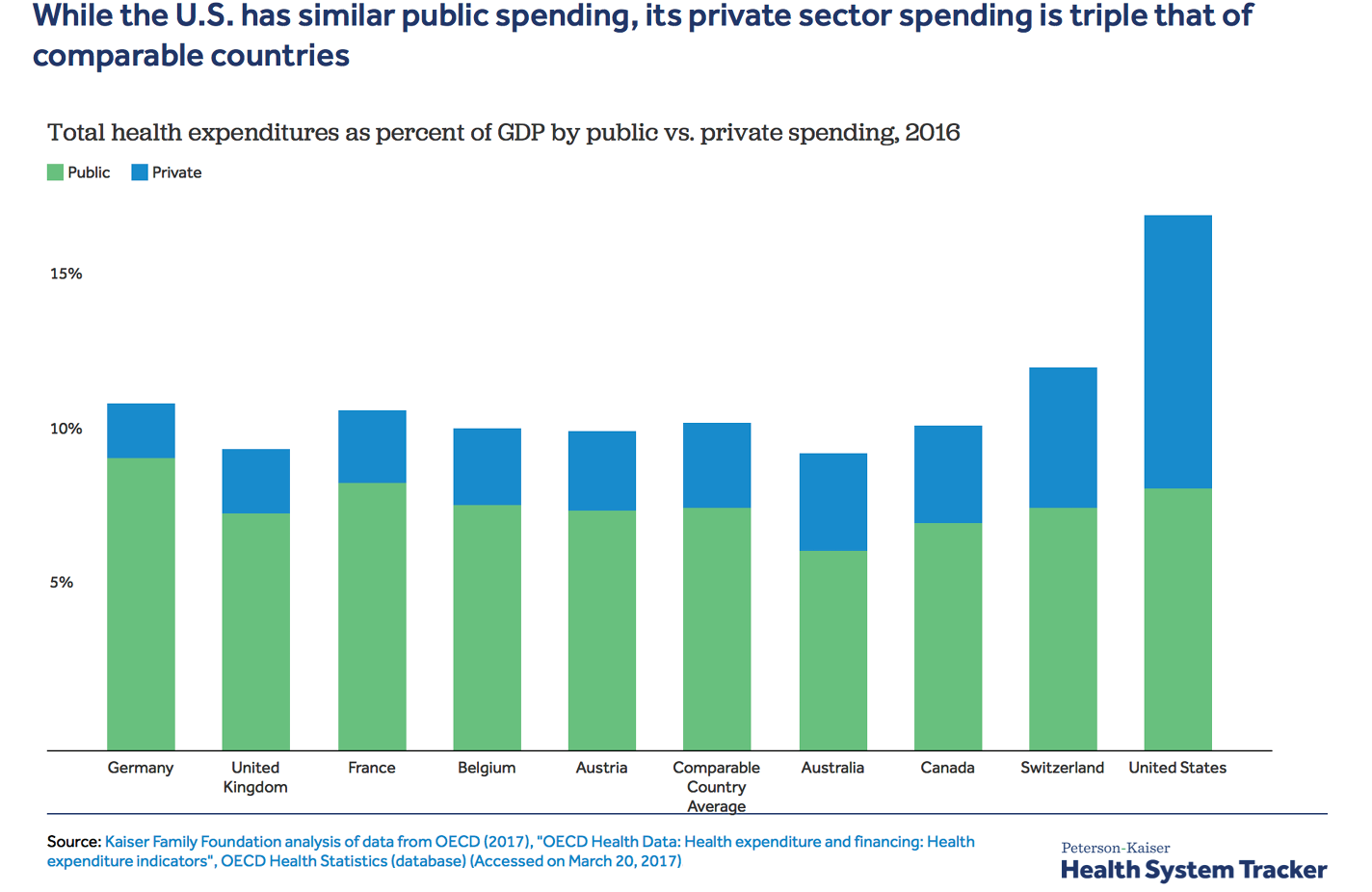
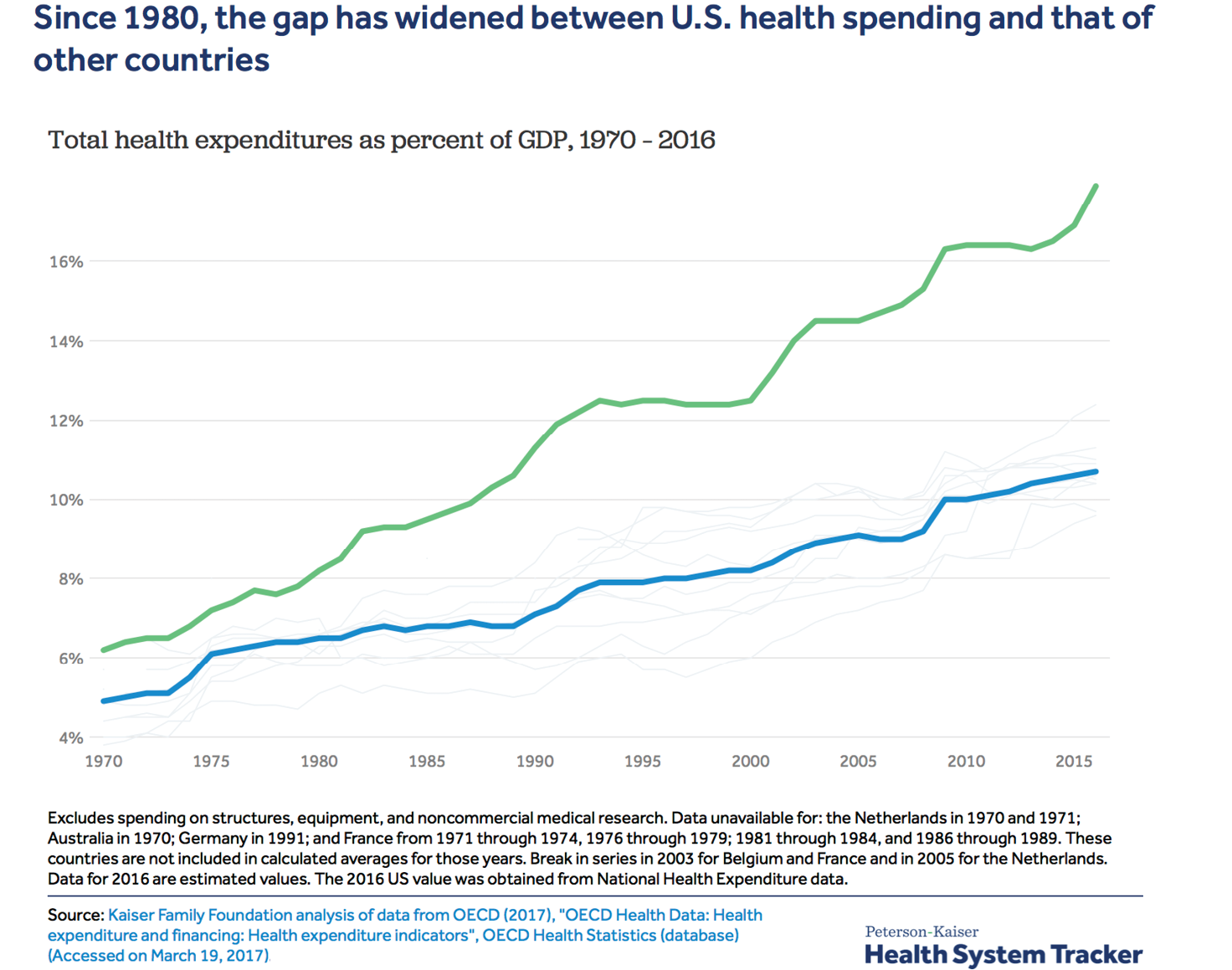
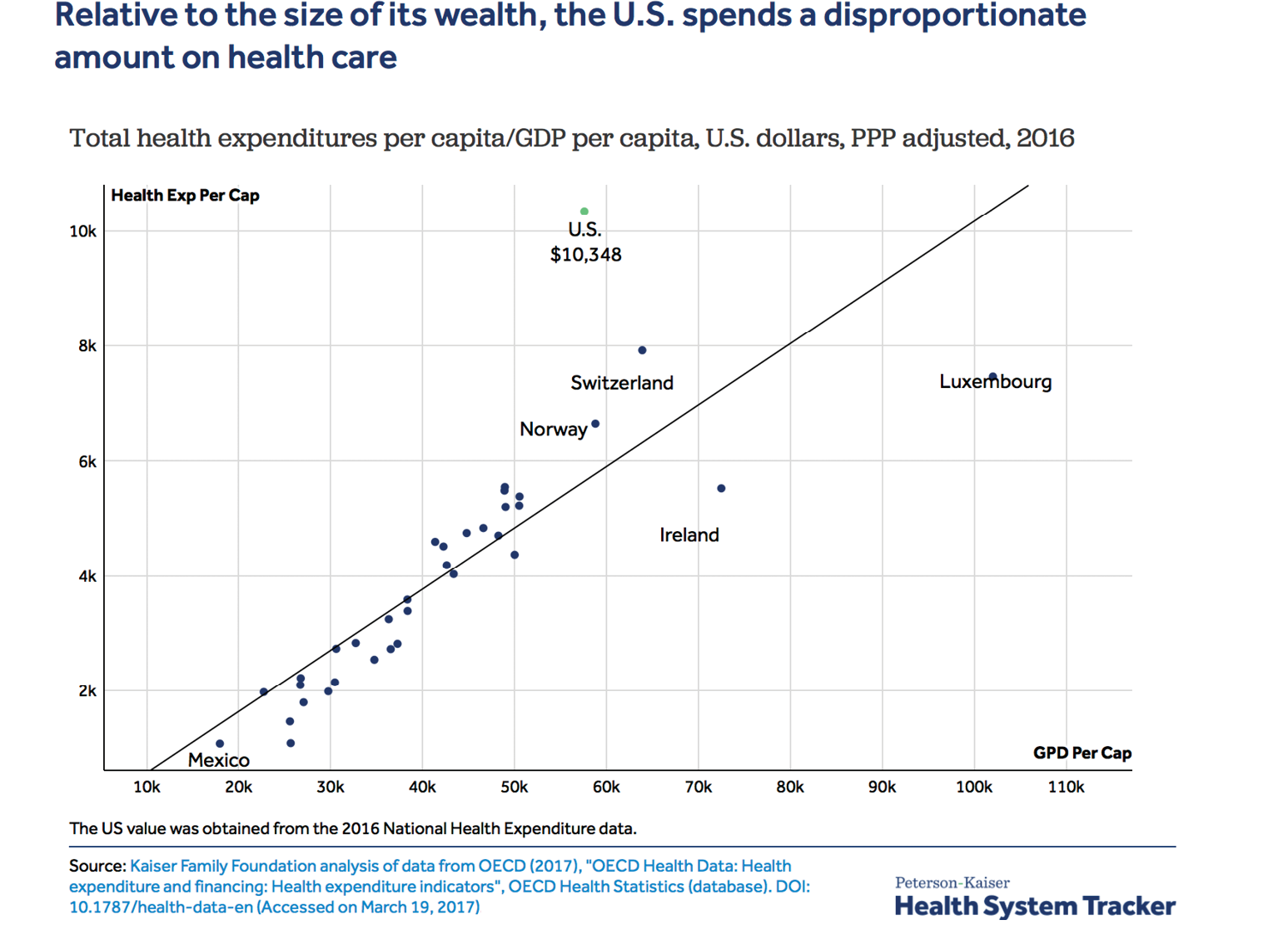
While the cost of health care has been increasing globally, the issue has been particularly acute in the U.S. There, health care reached over 17% of GDP in 2018 compared to 10% or less of GDP in comparably developed economies CMS OECD. All said, the cost of health care as a percentage of GDP has increased rapidly in the U.S., tripling in the last 50 years.
But all the extra money going to medical care is doing little to purchase health or peace of mind. Doctors are hamstrung by student debt and at the mercy of malpractice suits; patients fear being denied treatment Hoffower Guardian.
MEDICAL MONOPOLY AND THE NUMBER OF DOCTORS
This unsustainable cost increase results, to some extent, from the burden of an aging population as well as the cost of more advanced drugs. But it is also, if not mainly, a result of bad incentive structures either imposed by the state or tolerated by it. These structures inflate health care costs and thus put at risk the very preservation of a healthy social system JAMA Harvard Business Review.
Much of this can be attributed to what, as in real estate, can best be described as a structural market abuse. Some types of market abuse, such as restricting the supply of doctors, come from the authorities, be they public, that is the state, or private, that is the medical associations that are empowered by the state.
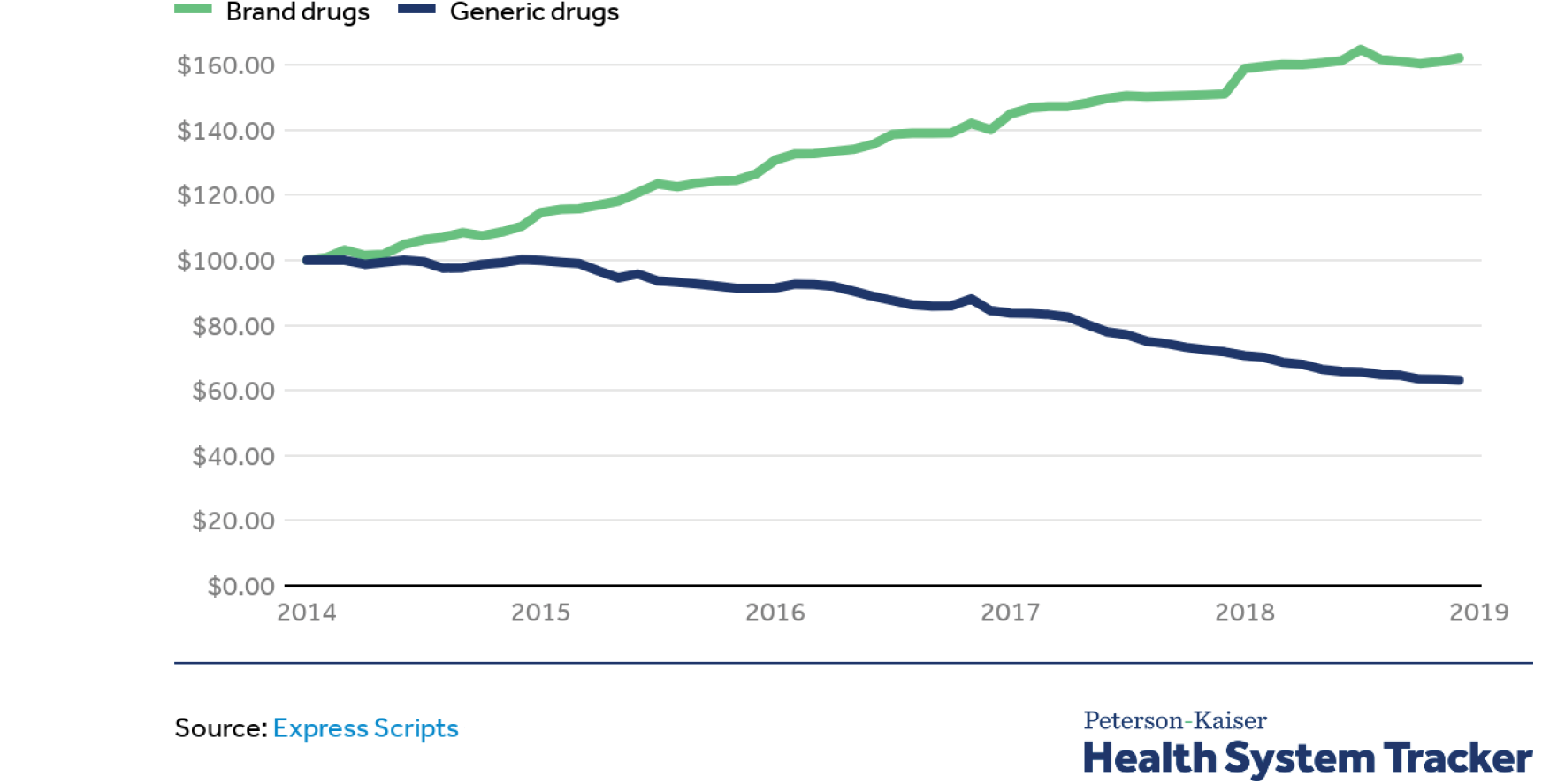
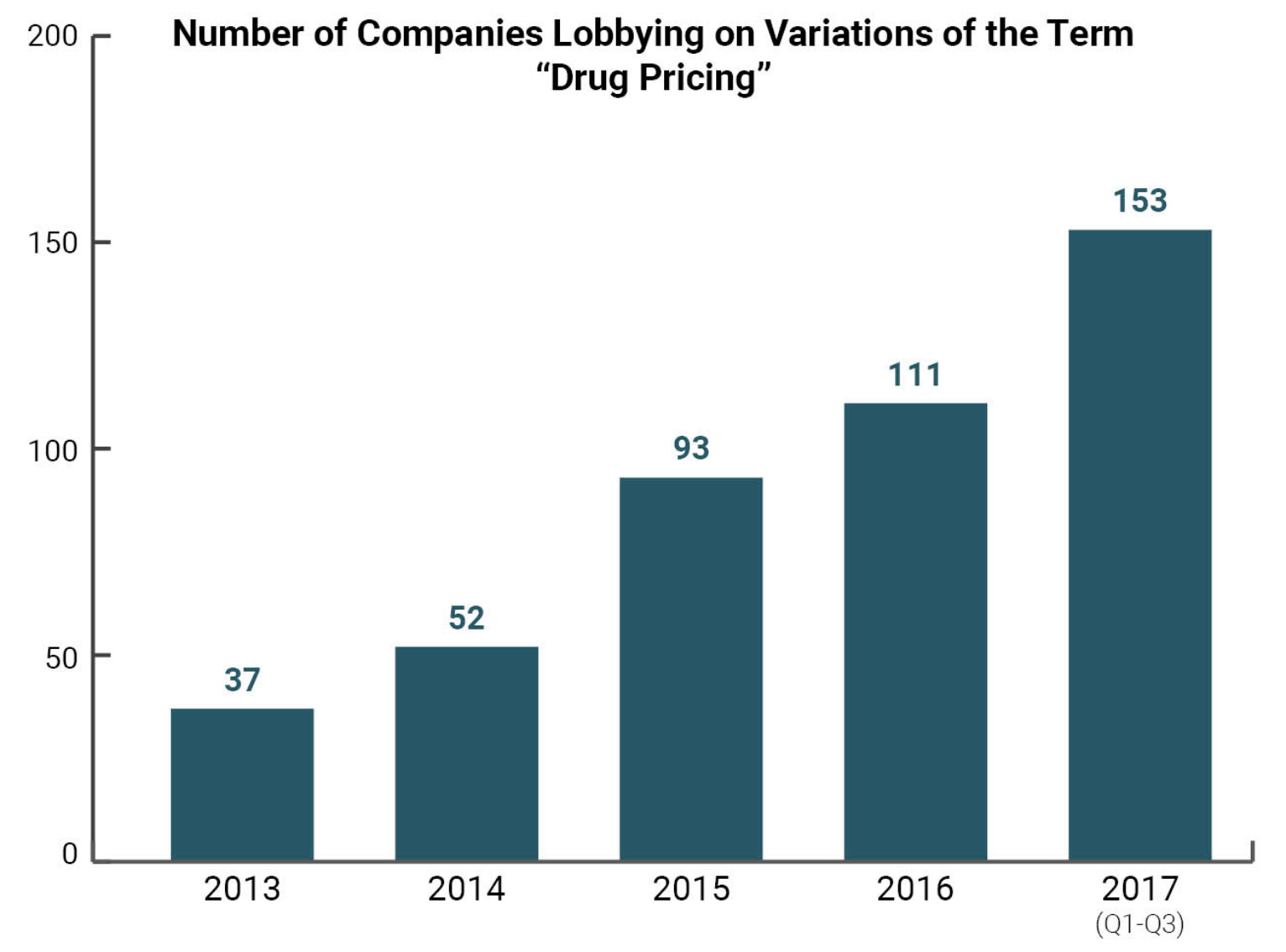
Market abuse can also come from private companies, such as pharmaceutical companies, which can freely set insane prices for the drugs they hold patents for, setting the stage for an aggressive monopolist pricing where the stakes can be life or death. And if they don’t hold the patents? Big Pharma will not let a thing like that stop them. Attorneys General in several U.S. states are currently suing more than a dozen generic drug companies for colluding to set the prices of over 300 drugs. The system is truly rigged.
SETTING THE NUMBERS OF DOCTORS
As with all goods and services, there is an intricate relationship between the number of doctors, the numbers of hours they work to supply medical assistance, and the price of this service.
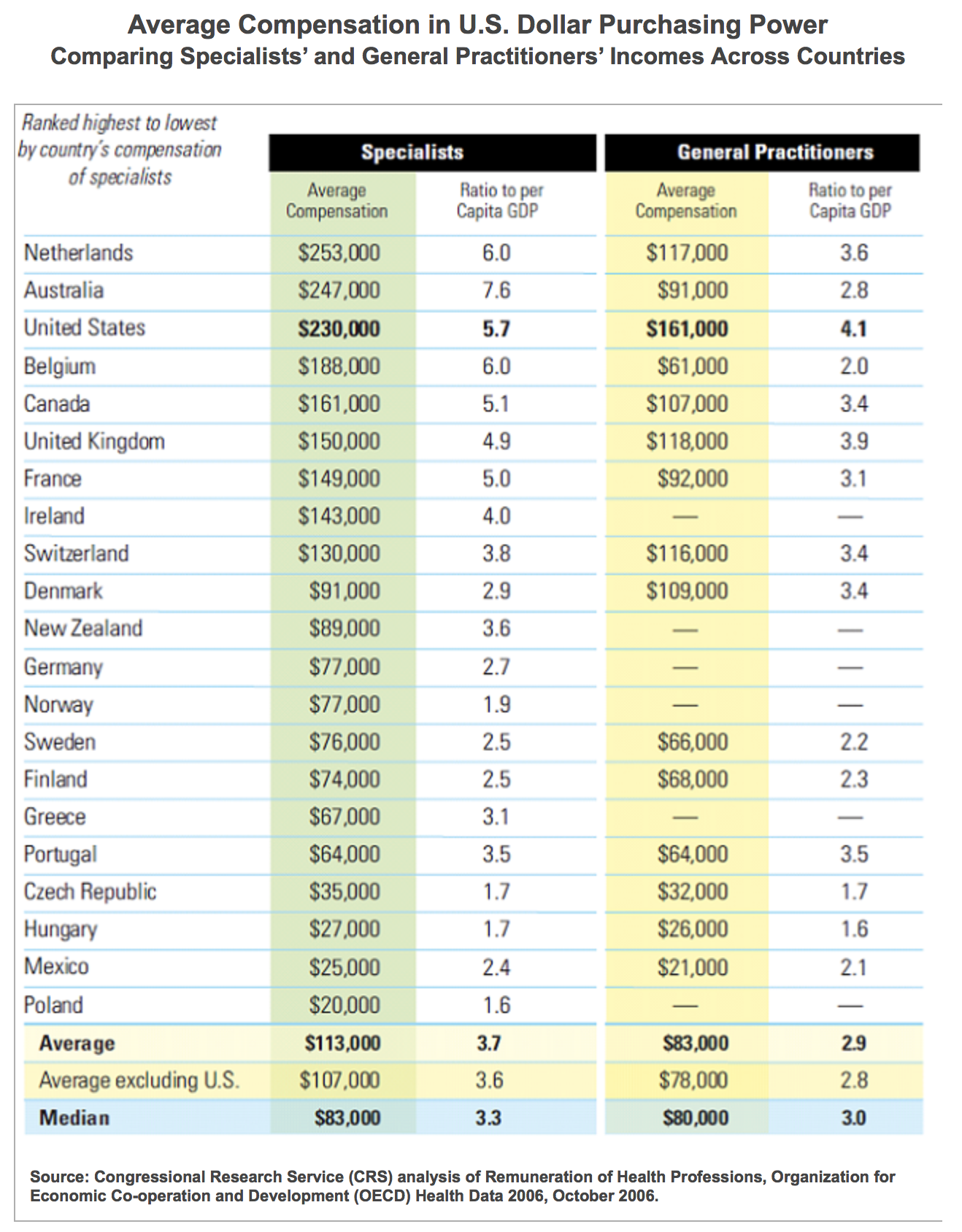
In the U.S., the number of doctors is arbitrarily decided by doctors themselves through the American Medical Association. A monopolist supplier, if allowed to set the level of production capacity, will always set it at a level below market equilibrium, creating a shortage that allows it to demand an exorbitant price. In the U.S., it results in an abnormally low number of generalists, which translates into generalists’ remuneration of close to four times the median wage, an international record Foundation for Economic Education.
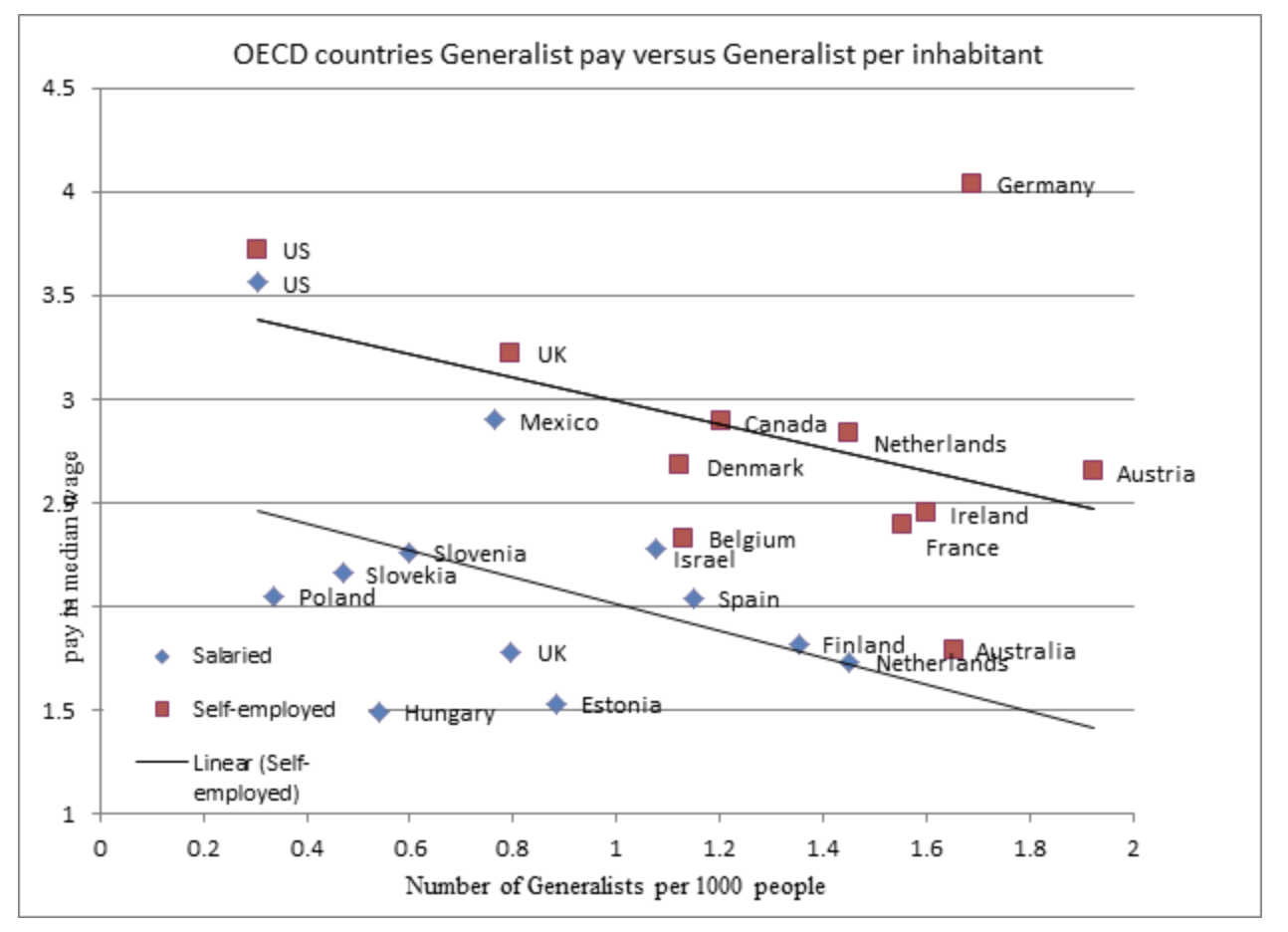
An interesting counterexample is given by the U.K. where doctors are also in short supply, but the “gain” is captured by the state. According to the OECD, the number of doctors per inhabitant in the U.K. is among the lowest in Europe, together with Poland, Romania and Slovenia. At 1.8 times the median wage for a generalist, they are also among the lowest paid. With limited pay and long working hours, U.K.-trained doctors are under pressure and there have been numerous reports of dissatisfaction and increased emigration by doctors, particularly to Australia and New Zealand, where working hours are shorter Consultancy.
Others don’t want to leave the U.K. and opt to work part-time in the more lucrative private sector. Remuneration for doctors in private practice in the U.K. is in line with other countries where the number of doctors is relatively limited. For generalists, the low number of doctors translates into remuneration over three times the median wage. But the gap in the U.K. between self-employed (private) and salaried (public) remuneration for generalists is the highest reported by the OECD Office of Health.
Both in the U.S. and the U.K., the number of GPs and their remuneration structures are dysfunctional. In the U.S., the price for private doctors’ visits (their remuneration) is essentially freely set, but the number of doctors is artificially kept low by the medical doctors’ association. This is yet another example of the state letting a corporatist monopolist maximize its (collective) gain at the expense of public well-being. As Milton Friedman wrote, “Licensure has reduced both the quantity and quality of medical practice … It has forced the public to pay more for less satisfactory medical service.” But it has helped maximize doctors’ income Friedman, Capitalism and Freedom.
Similarly, in the U.K., the NHS monopoly captures the market premium for low supply by paying low fixed wages to an under-staffed but captive workforce. British patients may pay lower costs through the NHS, but as a result, a lower-than-optimal number of doctors are at work. In this case, it is mainly the collectivity that is capturing the monopolist rent – a rent that comes from extracting additional unpaid or underpaid working hours from young doctors who cannot yet establish a private sector practice. But the older doctor in private practice also benefits from higher private demand (people dissatisfied with overworked NHS doctors) and lower supply (not enough doctors).
If international comparisons are any guide, the market outcome, or the numbers of doctors that would be available if people were to decide how much they are willing to pay, would be higher per inhabitant than currently exists in either the U.S. or the U.K. For instance, the Netherlands has nearly twice as many generalists as the U.K. They are salaried at the same rate but command a materially lower premium when self-employed OECD. As a general rule, the higher the number of doctors, the lower the wage premium that private practice commands.
It is time for a rethink of how the number of doctors is determined. Neither a model in which doctors’ associations control the total number of available professionals in order to maximize their gain nor a state agency seeking to minimize costs is optimal. In the U.K., a freer licensure market would likely produce more doctors who are less overworked, earning the same or moderately more than the NHS pays today, with private practice earning less. In the U.S., it would reduce costs across the board. Training doctors does not come free, but what we are faced with is a set of systems that works like a monopoly in favor of well-established doctors, a state sanctioned rent extraction.
Increasing the supply of doctors where needed could be done by simultaneously providing for their study costs in exchange for agreeing to work in local clinics for underserved populations as a salaried employee for some years. Community clinics should be shielded from most malpractice lawsuits, but patients could be offered, if they want, to take supplementary insurance to cover the costs of complications from procedures they undergo above certain fixed levels. As long as someone pays his or her study costs and demonstrates a sufficient level of qualification, there is no valid reason to bar that person from being a medical doctor. As a general rule, more should be done to increase the number of doctors, including addressing doctors’ reasonable concerns about student debt and malpractice suits.
PHARMACEUTICAL COMPANIES: RESEARCHING OR MARKETING?
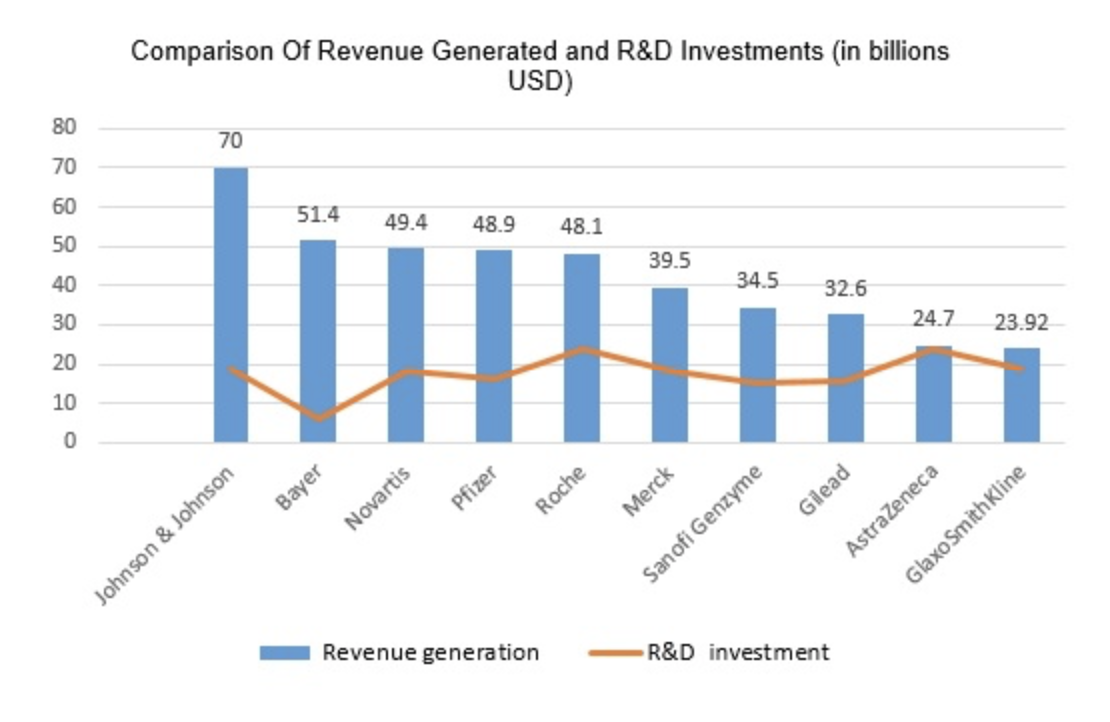
Pharmaceutical costs account for an ever-increasing portion of healthcare costs. The story spun out to justify this is that the research and development of new medicines is extremely expensive and risky. There is, of course, some truth in that. Indeed, in the United States, the largest supplier of drugs in the world, around 18% of revenue is dedicated to R&D. In the E.U., only about 10-15% of revenue goes to R&D TTconsultant.
Here’s the part of the story the pharmaceutical companies don’t talk about: They now spend twice as much money marketing their drugs to doctors and impressionable consumers than they spend on developing new ones York University.
They do this in part to brand their drugs in order to fend off the threat posed by generic rivals when their patents expire. They also try to boost demand for their product, by engaging in active promotion to doctors and would-be patients in an effort to promote pharmaceutical consumption, a practice which inevitably leads to over-medication. Patients are pushed to consume particular pharmaceutical products they have no understanding of through elaborate marketing, including TV advertisements relentlessly telling seniors to ask for specific medications from their doctors. Authorized in the U.S. only since 1998, pharmaceutical TV campaigns have exploded in recent years. From 2012 to 2016 alone, TV and advertisement by media companies has doubled, the number of ads increasing by 65% New York Times.
Big Pharma has also been known to twist patents in an effort to extend them and prevent generics from hitting the market, a practice that has become known as “evergreening.” 78% of new drug patents recorded by the FDA between 2005 and 2015 were awarded to existing drugs rather than new medications. 80% of the top 100 best-selling drugs have had their patent extended, 50% more than once. Throughout the industry, research indicated that companies “created serial barriers to hold off the type of competitive entry that is fundamental to our innovative system.” FiercePharma Feldman
The result of all this is that the profitability of pharmaceutical companies, as measured by their margins, is higher than car, oil and gas or media companies. These profits are the direct result of the ever-increasing prices charged to patients, their insurance companies, and governments Forbes.
The current system encourages overspending on marketing and abuse of the patent system rather than the much ballyhooed focus on costly R&D. In doing so, it contributes increasingly to exploding health care costs, severely affecting the most constrained among us. This is about segment monopolists propping up an inflated demand while limiting supply, in a typical market abuse behaviour. This behaviour is increasingly tolerated by the states that should regulate the pharmaceutical market like no other.
Like the American civil rights icon Fannie Lou Hamer, patients across the developed world are sick and tired of being sick and tired. And they’re sick of overpaying for that particular privilege, too.